When it comes to treating liver cancer, surgeons still are working “in the dark”.
Despite being the largest vital organ in the body, the liver has very few identifiable landmarks to help guide surgeons around its surface. Two-dimensional ultra-sound images currently are the standard navigational tool, making it difficult to discern depth and three-dimensional space during surgery.
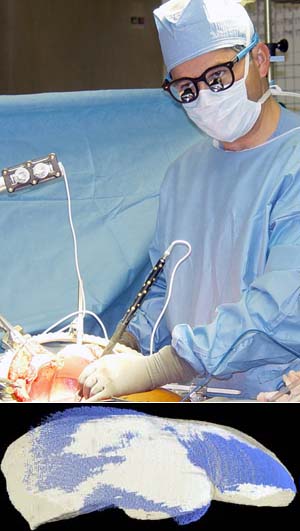
That’s why a research team at Washington University School of Medicine in St. Louis is launching two trials examining the use of three-dimensional imaging techniques to complement ultra-sound during liver surgery.
“These projects emphasize the strengths of this medical center,” says William C. Chapman, M.D., professor of surgery and chief of the Abdominal Transplantation Section at the School of Medicine. “The renowned Mallinckrodt Institute of Radiology and our surgical team’s expertise in treating liver cancer combine to provide a unique environment for exploring the application of three-dimensional modalities for liver surgery.”
One trial, funded by a three-year, $1.2 million grant from the National Cancer Institute, will examine the use of standard three-dimensional imaging techniques like magnetic resonance imaging (MRI), computed tomography (CT) and positron emission tomography (PET) for guiding surgeons during tumor removal or ablation surgery.

Imaging methods like MRI, CT and PET already are used to identify the location of liver tumors during diagnosis, but they cannot be used actively during surgery.
“Imaging plays a critical role in the evaluation and management of patients with liver problems, yet we still haven’t learned how to best translate the improvements in imaging technology for improvements in liver surgery,” Chapman explains. “In the same way that image-guided breast surgery now allows precise, minimally invasive biopsies and surgeries, our concept, if successful, would facilitate more precise use of current and future imaging technology for liver surgery.”
Chapman, who formerly was at Vanderbilt University, developed the basic components necessary to use three-dimensional imaging in the liver with an interdisciplinary team of scientists in Nashville. They developed surgical instruments, each with infrared light-emitting diodes scattered along the instrument’s handle. Three camera sensors are calibrated to detect the light from each diode in space and in relation to the tip of the instrument. Once properly calibrated, the cameras then can track the instrument tip’s movement by following the movement of the diodes.
Chapman’s team at Washington University recently completed a pilot study that demonstrated the method is feasible and safe to use in humans. Their new grant will allow the group to test the system’s accuracy in targeting tumors.
According to Chapman, targeting accuracy is key for treating liver cancer, particularly in light of recent advances in surgical treatments. Previously, liver tumors typically were cut away, but now surgeons also are able to ablate, or destroy, the diseased tissue. While it’s possible to examine excised tissue to ensure the entire tumor has been removed, it’s impossible to check that an entire tumor has been destroyed during ablation surgery. Improvements in navigational acuity provided by three-dimensional imaging could significantly enhance the accuracy and success of tumor ablation techniques and assist in procedures such as live donor liver transplantation.
The team’s second trial, funded by a $40,000 grant from the Siteman Cancer Center at the School of Medicine and Barnes-Jewish Hospital, will test a new type of radiolabeled PET tracer in patients with primary liver cancer.
To obtain a PET image, a tracer that lights up when imaged, called fluorodeoxyglucose, is injected into the bloodstream. Because different types of cells absorb different amounts of the tracer, tumor cells can be detected. But this standard PET tracer fails to catch up to one half of all tumors. Preliminary studies in Hong Kong, however, found that an alternative tracer called carbon-11-acetate is significantly more accurate.
“There are only about five places in the country that produce carbon-11-acetate, and Mallinckrodt Institute of Radiology is one of them,” Chapman says. “We couldn’t be doing this research anywhere else in this part of the country.”