Researchers may be a step closer to understanding what causes cataracts and what may help to prevent them.
In a new study published in the American Journal of Ophthalmology, researchers at Washington University School of Medicine in St. Louis report the culprit may be oxygen.
They measured oxygen concentrations in the eyes of patients undergoing retinal surgery. When a person has retinal surgery, standard practice calls for removal of the vitreous gel, a clear, jelly-like structure in the center of the eye. This removal, called a vitrectomy, makes it easier for surgeons to reach and repair the damaged retina.
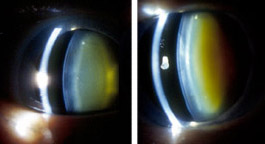
After vitrectomy surgery, the surgeon replaces the vitreous gel with fluid. But not long after that, the eye begins to develop the clouding of the lens known as a nuclear cataract. Cataracts are the most common cause of blindness in the world, accounting for nearly 50 percent of all blindness. In the United States where treatment is routine, surgical removal of cataracts and implantation of replacement lenses is the most expensive item in the Medicare ophthalmology budget, costing more than $5 billion annually.
“It’s fairly well-accepted in the field that anyone over the age of 50 who has vitrectomy surgery will develop a cataract within two years,” says Nancy M. Holekamp, M.D., a retina surgeon at the Barnes Retina Institute and the study’s lead author. “It’s a complication retina surgeons accept because vitrectomy surgery is so important to preserving vision in patients with retinal problems. But if we could understand this process and prevent it, patients would be better off.”
Just before surgery, Holekamp, an associate professor of clinical ophthalmology and visual sciences, measured oxygen levels adjacent to the lens and near the center of the eye in the vitreous gel of 69 eyes. Before retinal surgery, oxygen concentrations were very low in both places. After surgery, oxygen levels in both locations were about eight times higher than normal.

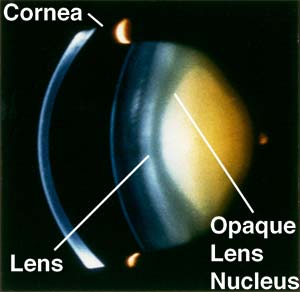
Although the retina has many blood vessels and high oxygen concentrations, the lens, separated from the retina by the vitreous gel, normally gets very little oxygen. After surgery, however, oxygen from the retina can migrate toward the lens because the replacement fluid used to replace the vitreous gel doesn’t prevent that movement the way the natural gel does.
“It seems one of the important functions of the vitreous gel is to keep oxygen away from the lens,” Holekamp says. “When we remove the gel, we remove that protective mechanism.”
Even after the vitreous gel has been removed, Holekamp says it may be possible to lower the amount of oxygen near the lens by lowering the oxygen level in the fluid that is pumped into the eye.
“We’re proposing that we deoxygenate the fluid used to replace the vitreous gel,” she says. “There’s no good reason to infuse such a highly oxygenated fluid into the eye. In fact, if we want to perform surgery under more natural conditions, we should remove the oxygen from that fluid.”

A co-investigator, David C. Beebe, Ph.D., the Janet and Bernard Becker Professor of Ophthalmology and Visual Sciences and professor of cell biology and physiology, believes the same kind of mechanism may contribute to cataracts that form as people age. The difference is that in age-related cataracts, the gel breaks down over several years. In vitrectomy patients, the gel disappears all at once.
The idea that breakdown of the vitreous gel might be related to risk for cataracts first was suggested in 1962 by a New Jersey ophthalmologist who noticed that many of his patients with nuclear cataracts also had degeneration of the vitreous gel. But this suggestion was not pursued, and it was more than 40 years before Beebe and colleague Ying-Bo Shui, M.D., Ph.D., a staff scientist in ophthalmology, demonstrated a statistical relationship between breakdown of the vitreous gel and the risk for cataracts.
They believe that when the gel separates from the retina or begins to break down and liquefy, it allows fluid to flow over the surface of the oxygen-rich retina and carry that oxygen to the lens. That’s true whether a person’s vitreous has begun to liquefy with age — a process known as vitreous liquefaction — or the vitreous gel has been removed in retinal surgery patients.
In past research, Beebe and his colleagues examined eyes that were donated to an eye bank. They found that the vitreous gel was almost completely intact in some eyes. The incidence of nuclear cataracts was very low in those eyes. But in other eyes, Beebe’s team found the vitreous gel had broken down and was more liquid. Those eyes had a much higher incidence of cataracts.
The vitrectomy study also taught Beebe and Holekamp that some retinal diseases may protect patients from cataracts. For example, patients who had retinal surgery for complications of diabetes had significantly lower levels of oxygen near the lens. They plan a follow-up study of whether diabetic patients are somehow protected from cataracts.
They also note that researchers in Japan have performed retinal surgery without removing the vitreous gel. The surgery is more difficult to do, but the Japanese team found that when the vitreous gel remains intact, retinal surgery patients don’t develop nuclear cataracts to the same extent.
Holekamp isn’t proposing retinal surgeons stop doing vitrectomies, but she says lowering oxygen concentrations in the fluid that replaces the vitreous gel might help protect the lens. She and her colleagues plan to investigate methods to do so. Beebe, too, is planning to conduct animal studies to see if he can prevent oxygen from reaching the lens.
“If we can remove or reduce the amount of molecular oxygen that reaches the lens, and that turns out to protect against nuclear cataracts in either human patients or in animals, I think it will make a very strong case for oxygen being the culprit,” he says.
Beebe, Holekamp and Ying-Bo Shui are launching a new Clinical Cataract Research Center at Washington University School of Medicine. They plan to study both the cataracts that form rapidly in vitrectomy patients and, in future studies, to look at drugs that may slow the onset or progression of cataracts.
“Perhaps we could replace the vitreous gel with a gel polymer that would keep oxygen away from the lens,” Beebe says. “Now that we’re beginning to get an idea of how the vitreous gel works, it may be possible to design interventions to protect the lens both in people who have had a vitrectomy and in those whose vitreous is degenerating as a part of normal aging.”
Holekamp NM Shui YB, Beebe DC. Vitrectomy surgery increases oxygen exposure to the lens: a possible mechanism for nuclear cataract formation. American Journal of Ophthalmology, vol. 139, pp. 302-310, Feb. 2005.
This research was supported by grants from Research to Prevent Blindness and the National Eye Institute of the National Institutes of Health.
The Clinical Cataract Research Center was made possible by the Dennis L. Gierhart Charitable Gift Fund.
The full-time and volunteer faculty of Washington University School of Medicine are the physicians and surgeons of Barnes-Jewish and St. Louis Children’s hospitals. The School of Medicine is one of the leading medical research, teaching and patient care institutions in the nation, currently ranked third in the nation by U.S. News & World Report. Through its affiliations with Barnes-Jewish and St. Louis Children’s hospitals, the School of Medicine is linked to BJC HealthCare.