Cancer cells get a helping hand from platelets, specialized blood cells involved in clotting. Platelets shelter and feed tumor cells that stray into the bloodstream, making it easier for cancer to spread, or metastasize. Research at Washington University School of Medicine in St. Louis suggests that inactivating platelets could slow down or prevent metastasis.
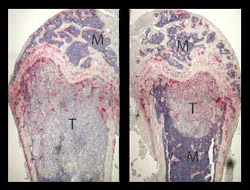
In advance online publication in the Journal of Cellular Biochemistry, the scientists report that a combination of two platelet inhibitors reduced the number and size of breast cancer or melanoma tumors that grew in the bones of laboratory mice. One of the drugs was aspirin, a widely used inhibitor of platelet clotting. The other was an experimental drug, APT102, which also prevents platelet clotting, but by a different mechanism. Both drugs were needed to reduce bone tumors.
“Past research has shown that tumor cells activate platelets and that mice with defective platelets have significantly fewer metastases,” says Katherine Weilbaecher, M.D., assistant professor of medicine and of cell biology and physiology. “We also know that platelets have several traits that can aid tumor cells, and we are working to break up that potentially lethal partnership.”
Metastasis of cancer cells to sites away from the main tumor can cause pain and other symptoms and greatly increases the likelihood a patient will die of the disease. In fact, more than 90 percent of cancer deaths are the result of metastasis, which is difficult to control with current therapies.
Cancer cells that leave the primary tumor and circulate in the bloodstream can readily take advantage of platelets they encounter. The circulating tumor cells secrete factors that make platelets stick together, creating a shield of platelets that protects cancer cells from immune attack. In addition, platelets release growth factors that help tumor cells survive, and platelets’ capacity to stick to particular sites enables companion tumor cells to settle in and proliferate in new areas.
Weilbaecher, an oncologist with the Siteman Cancer Center at Washington University School of Medicine and Barnes-Jewish Hospital, and colleagues, including Özge Uluçkan, a predoctoral trainee in molecular genetics, and Mark Eagleton, a research technician, tested the effect of aspirin and APT102 in mice that received an injection of either melanoma or breast cancer cells.
The cancer cells establish themselves in bones in as little as two days and proliferate to produce large bone tumors in less than two weeks. But the researchers found the bone tumors were smaller and fewer in mice that got a dose of aspirin and APT102 before inoculation with cancer cells and additional treatments twice a day for two days after that.
“We only had a small amount of APT102 to test, so in this set of experiments, we gave only a few doses of the drugs to the mice,” Uluçkan explains. “At this point, we don’t know if additional treatment would have further reduced the tumor burden, but it’s clear that reducing platelet function had a positive result in this model of metastatic cancer.”
By themselves neither aspirin nor APT102 lessened the amount and size of bone tumors in the mice, possibly because cancer cells can activate platelets in several different ways, making a dual approach more effective, according to Weilbaecher.
“Aspirin prevents platelets from making thromboxane, a substance that facilitates clotting,” Weilbaecher says. “APT102 is an especially interesting drug because it gets rid of a compound called ADP, which tumor cells release and which stimulates platelets to clump. So APT102 prevents platelet activation in response to tumor cells.”
APT102 is produced by APT Therapeutics Inc., a St. Louis-based biopharmaceutical company. The company donated the drug but did not fund the research project. Co-authors Soon Seog Jeong and Ridong Chen are employees of APT Therapeutics and provided expertise about the bioactivity and dosing of APT102.
The researchers noted that the drug combination would likely be well tolerated because it did not cause excessive bleeding in the mice, as might be expected from platelet inhibitors. The research group plans to continue to study the process of metastasis and the role played by platelets.
In collaboration with Michael Naughton, M.D., assistant professor of medicine, Weilbaecher is also involved in a clinical trial of women with advanced breast cancer to test aspirin and Plavix®, another antiplatelet drug, to see if the drug combination affects the number of tumor cells that circulate in the blood. The trial is open only to breast cancer patients undergoing treatment at the Siteman Cancer Center.
Uluçkan Ö, Eagleton MC, Floyd DH, Morgan EA, Hirbe AC, Kramer M, Dowland N, Prior JL, Piwnica-Worms D, Jeong SS, Chen R, Weilbaecher K. APT102, a novel adpase, cooperates with aspirin to disrupt bone metastasis in mice. Journal of Cellular Biochemistry, Feb. 7, 2008 (advance online publication).
Funding from National Institutes of Health, the Ewing Marion Kauffman Foundation, the Barnes-Jewish Hospital Foundation and Washington University supported this research.
Washington University School of Medicine’s 2,100 employed and volunteer faculty physicians also are the medical staff of Barnes-Jewish and St. Louis Children’s hospitals. The School of Medicine is one of the leading medical research, teaching and patient care institutions in the nation, currently ranked fourth in the nation by U.S. News & World Report. Through its affiliations with Barnes-Jewish and St. Louis Children’s hospitals, the School of Medicine is linked to BJC HealthCare.
Siteman Cancer Center is the only federally-designated Comprehensive Cancer Center within a 240-mile radius of St. Louis. Siteman Cancer Center is composed of the combined cancer research and treatment programs of Barnes-Jewish Hospital and Washington University School of Medicine. Siteman has satellite locations in West County and St. Peters, in addition to its full-service facility at Washington University Medical Center on South Kingshighway.