Walking, jogging and other forms of regular aerobic exercise may actually ward off the onset of Alzheimer’s disease pathology in the brain, suggests newly published research from Washington University in St. Louis.
In a study of 69 adults ages 55-88, WUSTL scientists examined the association between exercise habits and the presence of Alzheimer’s disease’s biological markers, or biomarkers. These biomarkers reflect the levels of certain proteins in the brain and spinal fluid that are characteristic of the brain pathology of Alzheimer’s.
Altered amounts of these proteins in the brain and spinal fluid may indicate the presence of the disease before symptoms appear.
The Alzheimer’s Association recommends physical activity to possibly preserve cognitive function or quality of life in diagnosed patients. Studies in mice models also suggest that exercise may reduce the accumulation of specific disease-associated proteins in the brain.
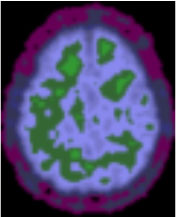
Brain image from an individual with higher exercise engagement and lower amyloid deposition.
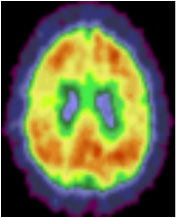
Brain image from an individual with lower exercise engagement and higher amyloid deposition.
But the WUSTL study, published in the September 2010 issue of Annals of Neurology, is a unique demonstration in humans of a relationship between physical activity and the biomarkers for Alzheimer’s, according to Denise Head, PhD, assistant professor of psychology in Arts & Sciences.
“This novel association, in conjunction with the animal work, suggests that it may be useful for physicians to recommend exercise engagement not only for Alzheimer’s symptoms but also potentially for preventative care,” Head says. “We have not researched to the point where it can be proven that exercise helps prevent Alzheimer’s symptoms, but that’s the direction we’d like to go.”

Head
Heading off a crisis
The study volunteers, all of whom had normal cognition, filled out questionnaires about their exercise habits during the previous 10 years. Researchers then analyzed the participants’ cerebrospinal fluid samples and PET scan images of a brain protein called amyloid that accumulates as “plaques” in the brains of Alzheimer’s patients.
To measure activity levels, the scientists used the American Heart Association (AHA) guideline: 30 minutes of moderate exercise five days a week.
The investigators discovered that volunteers who exercised at levels near to or greater than those recommended by the AHA over the past decade had decreased levels of amyloid in the brain as well as suggestions of lowered levels of another protein called tau, a marker of dysfunction and/or death of neurons.
This finding is critical to efforts toward curbing a potential public health crisis. Today, 4.5 million Americans have Alzheimer’s disease, a number expected to climb to 13.2 million by 2050.
The national cost for 2010, a predicted $172 billion, could soar to more than $1 trillion by the mid-century mark.
“With the growing aging population in the U.S., Alzheimer’s is going to become an increasingly prevalent disease affecting many families and taking a significant financial toll,” says Kelvin Y. Liang, Head’s MD/PhD student and lead author of the study.

Liang
“Because the disease has a such a long timeline, we’re looking at a lot of lifestyle and other factors, such as exercise, that could prevent the disease before it gets to the stage where you have clinical symptoms — where there may not be as much you can do about it,” Liang says.
Next steps
The research team also included Mark A. Mintun, MD, chief medical officer for Avid Radiopharmaceuticals Inc.; Anne M. Fagan, PhD, research associate professor of neurology; Alison M. Goate, PhD, professor of genetics, of genetics in psychiatry and of neurology; Julie M. Bugg, PhD, postdoctoral research associate in the Department of Psychology; David M. Holtzman, MD, the Andrew B. and Gretchen P. Jones Professor of Neurology and head of the Department of Neurology; and John C. Morris, MD, the Harvey A. and Dorismae Hacker Friedman Distinguished Professor of Neurology and director of the Charles F. and Joanne Knight Alzheimer’s Disease Research Center (ADRC).
The team doesn’t yet understand the exact mechanism by which exercise may affect Alzheimer’s biomarkers, but physical activity is known to have beneficial effects on regions of the brain, such as the memory-related hippocampus that is implicated in Alzheimer’s.
Exercise also has been associated with the creation of several important brain components, including neurons, blood vessels and chemicals that promote the health of neurons in the brain.
Furthermore, there may be a connection between improved cardiovascular health resulting from physical activity and conditions associated with Alzheimer’s, such as disturbances in insulin and glucose. Future research will use the same bank of study volunteers from the ADRC.
“Our study was a first step,” Head says. “Now there are two possible interpretations we need to tease apart: does exercise lead to lower amyloid deposition or does amyloid deposition lead to less exercise? Future studies also need to look at the influence of other relevant lifestyle factors that may interact with exercise engagement.”
As they plan upcoming studies, the investigators never lose sight of the fact that their science exists to serve people affected by Alzheimer’s.
“A researcher can be really focused on a particular part of a certain mechanism of this disease that he or she is studying, and that’s an important step in developing therapies and other diagnostic tests,” Liang says. “But in the end, we should always keep in mind that everything we do is to benefit the patient.”
Head, whose research focuses on the neural basis of cognitive aging, uses behavioral testing and both structural and functional neuroimaging in her study of aging in the healthy population and in those with Alzheimer’s.