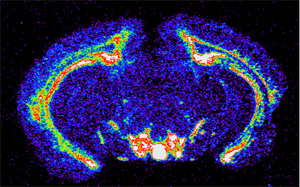
Jerry Stitzel, University of Colorado, Boulder
The CHRNA gene is active in brain areas linked to addiction. In this image from a mouse brain, the bright white areas are the brain regions in which the gene is highly active.
Your DNA influences how much you smoke and whether you will develop lung cancer or chronic obstructive pulmonary disease (COPD), according to an international team of researchers led by Washington University School of Medicine in St. Louis.
The study is the first large-scale effort to match genetics with smoking, lung cancer and COPD combined. The investigators studied 38,000 smokers and found that two groups of gene variants on chromosome 15 influence risk for all three problems. Their findings appear in the journal Public Library of Science (PLoS) Genetics.
“We put together a consortium from around the world and analyzed DNA variants that we know cause biological changes in smokers,” says the study’s senior investigator Laura Jean Bierut, MD. “We were able to demonstrate that both of the variants affect the amount a person smokes. Then we showed that the same pattern of variants contributes to lung cancer and COPD.”

Bierut
Nicotine, the main, addictive ingredient in cigarettes, binds to nicotinic receptors in cells. Past genetic studies had implicated a section of chromosome 15 that includes important nicotinic receptor genes, and in this study, the investigators looked specifically at those genes (CHRNA5, CHRNA3 and CHRNB4). Various forms of the nicotinic receptor genes were associated with how much a person smoked, and not surprisingly, heavy smokers turned out to be at greatest risk for lung cancer and COPD.
Bierut, a professor of psychiatry and principal investigator of the Collaborative Genetic Study of Nicotine Dependence, and Nancy L. Saccone, PhD, assistant professor of genetics and lead author of the study, joined forces with geneticists who study addiction, lung cancer and COPD as the Consortium for the Genetic Analysis of Smoking Phenotypes (CGASP). It is one of four consortia organized to study genetic data in smokers. All four groups have identified nicotinic receptor genes on chromosome 15 as important to smoking or lung disease.
“Previous studies have shown associations between gene variants and smoking,” Saccone says. “The important finding from our analysis is that a new group of variants also is associated with smoking behavior, further highlighting this area as an important target for follow-up studies to better understand the mechanisms underlying those associations we observed.”
The CGASP group took a different approach than the other groups. Scientists in the other groups simply surveyed the genome and looked for DNA regions that looked different in smokers. The CGASP study started with the hypothesis that cigarette smoking, lung cancer and COPD are linked at the genetic level and concentrated in particular on nicotinic receptor genes. But the two different approaches yielded similar results, finding that DNA differences on chromosome 15, particularly in the CHRNA5 nicotine receptor gene, made significant contributions to nicotine addiction, lung cancer and COPD.
Another difference between the various studies was that the CGASP group also looked at all three problems – nicotine addiction, lung cancer and COPD – rather than just one.
“Demonstrating that all three diseases are related to smoking behavior does not prove that there is a direct, biological effect linking nicotine addiction to cancer and COPD, but you certainly can’t rule it out,” Bierut says. “It’s really striking that this one gene is strongly driving addictive behavior and that it’s also related to lung cancer and COPD.”
The CHRNA5 gene functions both in the lung and in the brain. It is active in regions of the brain involved in addictive behavior.
“There’s a reward center in the brain,” Bierut says. “The center becomes activated with addiction, and the gene is clearly active in that brain region. But the gene also functions in the lung, meaning we need to ask the question of whether this gene is both driving the pathology of addiction in the brain while also working in the lung to contribute to COPD and cancer.”
She says the gene variants identified by the CGASP consortium don’t determine whether a person will smoke, but rather how much they will smoke, from light-smoking people who smoke fewer than 10 cigarettes per day to heavy smokers who light up more than more than 20 times daily. And how much an individual smokes is one of the strongest contributors to lung cancer and COPD.

Saccone
Depending on which gene variants a person has, that individual will tend to smoke different amounts. Bierut says people respond to nicotine differently, based in part on their genetic makeup, and then they adjust the amount they smoke according to nicotine’s addictive effects.
And Saccone says as the researchers continue to study the connections between genes, smoking, lung cancer and COPD, it will be important to pay close attention to the combined effects of small genetic variations.
“What we’ve identified in this study was detectable only after we accounted for the effects of other genetic variants in the same region of chromosome 15,” she says. “I think this study illustrates that important effects can be obscured unless we move beyond separate analyses of single gene variants to joint analyses of multiple variants.”
Saccone NL, et al. Multiple independent loci at chromosome 15q25.1 affect smoking quantity: a meta-analysis and comparison with lung cancer and COPD. PLoS Genetics, vol. 6 (8). Aug. 2010. www.plosgenetics.org.
Washington University School of Medicine’s 2,100 employed and volunteer faculty physicians also are the medical staff of Barnes-Jewish and St. Louis Children’s hospitals. The School of Medicine is one of the leading medical research, teaching and patient care institutions in the nation, currently ranked fourth in the nation by U.S. News & World Report. Through its affiliations with Barnes-Jewish and St. Louis Children’s hospitals, the School of Medicine is linked to BJC HealthCare.