Audio available
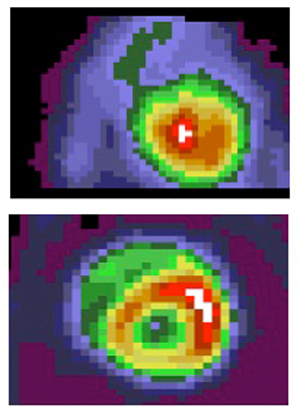
People with HIV often develop blood sugar and lipid problems and other metabolic complications that increase the risk of heart disease. But new research at Washington University School of Medicine in St. Louis shows that the HIV virus and the drugs used to treat it don’t worsen heart metabolism and function in these patients, compared with HIV-negative patients with metabolic complications.
The findings are reported online in the journal Cardiovascular Diabetology.
The researchers say the findings were surprising because metabolic complications like insulin resistance, diabetes and
problems with blood lipids — such as cholesterol, triglycerides and fatty acids — have become common as improved drug therapies enable
patients with HIV to live longer. These complications also tend to strike HIV-infected
people at a younger age. Scientists have long speculated that these
problems are caused either by the virus or the antiretroviral therapies
used to prevent the infection from progressing to full-blown AIDS.
The scientists used positron emission tomography (PET) imaging and echocardiography to study the heart in four groups of patients: 23 HIV-positive men with metabolic complications; 15 HIV-positive men without those problems; nine HIV-negative men with metabolic complications; and 22 HIV-negative men without them.
The PET studies measured how well the heart processes glucose, an indicator of how well the heart converts sugar into energy. The echocardiograms measured heart function, in particular the ability of the heart to relax between beats, known as diastolic function.
“We had thought that HIV-positive men with insulin and blood lipid problems would have the worst glucose utilization in the heart and the worst diastolic heart function,” says principal investigator W. Todd Cade, PT, PhD, assistant professor of physical therapy and of medicine. “But instead we found that HIV really didn’t make much difference. Men with these metabolic complications had impaired glucose utilization in the heart and poor diastolic function, regardless of HIV status.”
But the effectiveness of anti-HIV drugs may explain why heart function among HIV-positive men in this study was not worse than that of their HIV-negative counterparts, Cade says.

“We think HIV infection made little difference because the virus was so well controlled in the men we studied,” he says. “They had strong immune systems. If we had looked at patients with impaired immune systems and higher virus levels, we may have seen more heart problems.”
Cade says it’s possible that if a larger study were conducted, researchers may be able to tease out very small differences in heart function between HIV-positive and HIV-negative men.
“Our results suggest that men with metabolic problems should receive treatment, regardless of HIV status,” Cade says. “Whether you have HIV or not, insulin resistance and high blood lipids impair your heart’s ability to process nutrients, which over time can interfere with heart function, but our study showed that having
well-controlled HIV infection doesn’t make heart
metabolism and function any worse.”
Cade WT, Reeds DN, Overton ET, Herrero P, Waggoner AD, Davila-Roman VG, Lassa-Claxton S, Gropler RJ, Soto PF, Krauss MJ, Yarasheski KE, Peterson LR. Effects of human immunodeficiency virus and metabolic complications on myocardial nutrient metabolism, blood flow and oxygen consumption: a cross-sectional analysis. Cardiovascular Diabetology, Dec. 2011. (Epub ahead of print).
Funding for this research comes from the National Institute of Diabetes and Digestive and Kidney Diseases and the National Center for Research Resources of the National Institutes of Health (NIH), and the NIH Roadmap for Medical Research.
Washington University School of Medicine’s 2,100 employed and volunteer faculty physicians also are the medical staff of Barnes-Jewish and St. Louis Children’s hospitals. The School of Medicine is one of the leading medical research, teaching and patient care institutions in the nation, currently ranked fourth in the nation by U.S. News & World Report. Through its affiliations with Barnes-Jewish and St. Louis Children’s hospitals, the School of Medicine is linked to BJC HealthCare.