Audio available
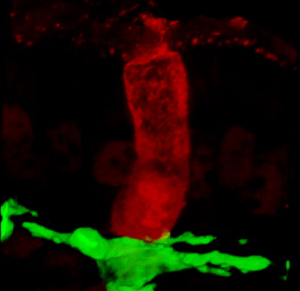
therapies against inflammatory bowel disease, celiac disease and food
allergies — disorders caused by an overactive immune system. Above, a sugar antigen ingested by a mouse fills a goblet cell (red) in the intestine, which delivers the antigen to a dendritic cell (green). Dendritic cells use the antigens to educate the immune system to recognize food antigens as harmless rather than as infectious agents. (Credit: Washington University School of Medicine )
With every meal, immune cells in the intestine stand like sentries at a citadel, turning away harmful bacteria but allowing vitamins and nutrients to pass.
Now, researchers at Washington University School of Medicine in St. Louis have identified the cells that chaperone food antigens, or proteins, in the intestine so that the immune system doesn’t mount an attack.
Their discovery, in mice, sheds new light on the function of goblet cells that line the intestine, and provides scientists with a potential target for therapies against inflammatory bowel disease, celiac disease and food allergies — disorders caused by an overactive immune system.
The researchers report their findings March 15, 2012, in the journal Nature.
“We found evidence that goblet cells work the same way in people and mice,” says co-principal investigator Rodney D. Newberry, MD. “We knew that if you eat a protein or antigen, it gets taken up in the intestine by immune cells called dendritic cells, and you become tolerant to it. But we didn’t know how the dendritic cells and the antigens got connected. From our experiments, it appears that goblet cells act as the matchmaker, bringing the food you eat and the dendritic cells together. That means goblet cells could become a hot target for new therapies.”
Using a novel imaging technique, the scientists watched the inner workings of the intestine in a living mouse in real time. They observed as antigens from a labeled sugar ingested by the mouse were passed by goblet cells to dendritic cells. (To see a video of dendritic cells, shown in green, in the intestine of a living mouse, click here.)
Dendritic cells play a key role in the immune system. But until now, scientists had thought that goblet cells in the intestine had only one job — to secrete mucus.
“Everyone has concentrated only on the fact that goblet cells secrete mucus, but I think in the face of our findings, you could perhaps wonder whether the problem in inflammatory bowel disease might result in part from goblet cells not delivering antigens to the correct place,” says Newberry, an associate professor of medicine in the Division of Gastroenterology. “Or maybe they’re not delivering antigens at all or too many antigens. We just don’t know yet.”
The small intestine is like a long, coiled tube. The center of that tube, the lumen, is filled with food material and bacteria that normally don’t cause disease. It’s protected from harmful pathogens by a layer of mucus secreted from goblet cells.
According to co-principal investigator, Mark J. Miller, PhD, assistant professor of pathology and immunology, antigens start out on one side of that mucus barrier while the immune system’s dendritic cells are on the other side. Miller and Newberry used a technique called two-photon imaging to watch as antigens were transported across that barrier.
“At any given time, there are goblet cells transporting antigens,” Miller says. “And that appears to be the mechanism to deliver food antigens and maybe even self-antigens to dendritic cells to induce tolerance. If the dendritic cells have access to antigens, they can educate T-cells that these are harmless antigens rather than infectious agents.”
He says the findings are important because now scientists know that immune responses in the intestine may depend as much on the ability of goblet cells to transport antigens to dendritic cells as on what the dendritic cells then do with the antigens. And Miller says no one knew that before because it only recently has become possible to watch intestinal immune cells in action in a living animal.
“This is not the role for goblet cells that we would have predicted,” Miller says. “But that’s the power of this type of imaging. Often, you’ll come across some new phenomenon that you didn’t expect. Sometimes, just by looking you realize there’s more to a system than you originally thought, and that leads you in new directions.”
Miller and Newberry also looked at healthy human intestinal tissue that had been removed from patients undergoing weight-loss surgery. It became clear from this work that goblet cells perform the same function in people as in mice, which raises the prospect that the cells may be valid drug targets for treating inflammatory bowel disease and other intestinal problems caused by an over-stimulated immune system.
In the current study, the researchers looked at mice that were normal and healthy, but the researchers are currently engaged in experiments in which they use the same imaging technique to look at how goblet cells and dendritic cells might function differently when inflammation or infection occurs. They also plan to study mucus-producing goblet cells in other tissues, such as the lung, to determine whether they are working the same way elsewhere in the body.
McDole JR, Wheeler LW, McDonald KG, Wang B, Konjufca V, Knoop KA, Newberry RD, Miller MJ, Goblet cells deliver luminal antigen to CD103+ DCs in the small intestine. Nature, vol. 483(7389), March 15, 2012.
Funding for this research comes from grants awarded by the National Institute on Diabetes and Digestive and Kidney Diseases and the National Institute of Allergy and Infectious Diseases of the National Institutes of Health (NIH) and by the Alvin J. Siteman Cancer Center at Barnes-Jewish Hospital and Washington University School of Medicine in St. Louis.
Washington University School of Medicine’s 2,100 employed and volunteer faculty physicians also are the medical staff of Barnes-Jewish and St. Louis Children’s hospitals. The School of Medicine is one of the leading medical research, teaching and patient care institutions in the nation, currently ranked fourth in the nation by U.S. News & World Report. Through its affiliations with Barnes-Jewish and St. Louis Children’s hospitals, the School of Medicine is linked to BJC HealthCare.