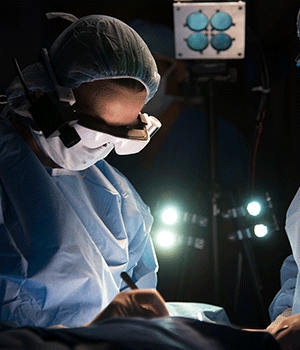
High-tech glasses developed at Washington University School of Medicine in St. Louis may help surgeons visualize cancer cells, which glow blue when viewed through the eyewear.
The wearable technology, so new it’s yet unnamed, was used during surgery for the first time Feb. 10 at Alvin J. Siteman Cancer Center at Barnes-Jewish Hospital and Washington University School of Medicine.
Cancer cells are notoriously difficult to see, even under high-powered magnification. The glasses are designed to make it easier for surgeons to distinguish cancer cells from healthy cells, helping to ensure that no stray tumor cells are left behind during surgery.
“We’re in the early stages of this technology, and more development and testing will be done, but we’re certainly encouraged by the potential benefits to patients,” said breast surgeon Julie Margenthaler, MD, an associate professor of surgery at Washington University, who performed the operation. “Imagine what it would mean if these glasses eliminated the need for follow-up surgery and the associated pain, inconvenience and anxiety.”
The current standard of care requires surgeons to remove the tumor and some neighboring tissue that may or may not include cancer cells. The samples are sent to a pathology lab and viewed under a microscope. If cancer cells are found in neighboring tissue, a second surgery often is recommended to remove additional tissue that also is checked for the presence of cancer.
The glasses could reduce the need for additional surgical procedures and subsequent stress on patients, as well as time and expense.
Margenthaler said about 20-25 percent of breast cancer patients who have lumps removed require a second surgery because current technology doesn’t adequately show the extent of the disease during the first operation.
“Our hope is that this new technology will reduce or ideally eliminate the need for a second surgery,” she said.

The technology, developed by a team led by Samuel Achilefu, PhD, professor of radiology and of biomedical engineering at Washington University, incorporates custom video technology, a head-mounted display and a targeted molecular agent that attaches to cancer cells, making them glow when viewed with the glasses.
In a study published in the Journal of Biomedical Optics, researchers noted that tumors as small as 1 mm in diameter (the thickness of about 10 sheets of paper) could be detected.
Ryan Fields, MD, a Washington University assistant professor of surgery and Siteman surgeon, plans to wear the glasses later this month when he operates to remove a melanoma from a patient. He said he welcomes the new technology, which theoretically could be used to visualize any type of cancer.
“A limitation of surgery is that it’s not always clear to the naked eye the distinction between normal tissue and cancerous tissue,” Fields said. “With the glasses developed by Dr. Achilefu, we can better identify the tissue that must be removed.”
In pilot studies conducted on lab mice, the researchers utilized indocyanine green, a commonly used contrast agent approved by the U.S. Food and Drug Administration. When the agent is injected into the tumor, the cancerous cells glow when viewed with the glasses and a special light.
Achilefu, who also is co-leader of the Oncologic Imaging Program at Siteman Cancer Center and a professor of biochemistry and molecular biophysics, is seeking FDA approval for a different molecular agent he’s helping to develop for use with the glasses. This agent specifically targets and stays longer in cancer cells.
“This technology has great potential for patients and health-care professionals,” Achilefu said. “Our goal is to make sure no cancer is left behind.”
Viktor Gruev, PhD, assistant professor of engineering at WUSTL, and Ron Liang, PhD, of the University of Arizona, assisted with development of the glasses. WUSTL graduate students Suman Mondal, Shengkui Gao and Yang Liu and postdoctoral fellow Nan Zhu also played key roles.
Comments and respectful dialogue are encouraged, but content will be moderated. Please, no personal attacks, obscenity or profanity, selling of commercial products, or endorsements of political candidates or positions. We reserve the right to remove any inappropriate comments. We also cannot address individual medical concerns or provide medical advice in this forum.