More than 50,000 surgical patients undergo general anesthesia every day in the United States, but clinicians and scientists lack evidence indicating which types of anesthesia drugs result in the best outcomes for patients.
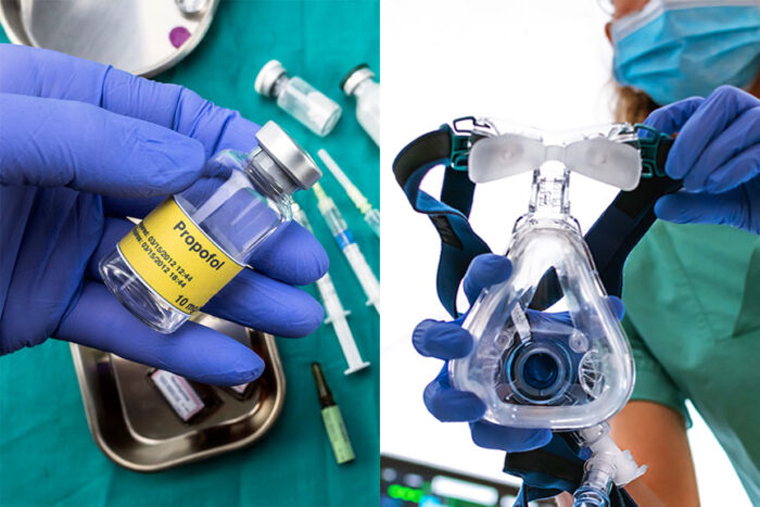
A new study led by researchers at Washington University School of Medicine in St. Louis and the University of Michigan will compare intravenous propofol to inhaled anesthetic drugs to determine which of the common anesthetic drugs offers better patient recovery experiences and improved clinical outcomes.
With a $33 million grant from the Patient-Centered Outcomes Research Institute (PCORI), the researchers will coordinate a study called THRIVE — Trajectories of Recovery After Intravenous Propofol vs. Inhaled Volatile Anesthesia. The 6½-year study will be conducted at clinical centers that are part of the Multicenter Perioperative Outcomes Group (MPOG), for which the University of Michigan is the coordinating center.
Other centers that are part of the MPOG group — including Washington University, the University of Pennsylvania, and Stanford University — will design and plan the study. About a dozen other MPOG clinical centers will enroll patients.
Sachin Kheterpal, MD, the associate dean for research information technology and a professor of anesthesiology at the University of Michigan and Washington University’s Michael Avidan, MBBCh, the Dr. Seymour and Rose T. Brown Professor and head of the Department of Anesthesiology, are the study’s principal investigators.
“General anesthesia is widely regarded as one of the most important medical advances in history, allowing millions to safely undergo invasive surgical procedures without suffering,” Avidan said. “The THRIVE trial is designed to answer fundamental questions regarding which of the two main anesthesia techniques provides a superior experience for patients during the recovery period, without compromising safety.”
Both intravenous propofol and inhaled anesthetic drugs have been in use for many decades. Both techniques have well-established records of safety and efficacy, and both are used every day in surgical procedures performed across the country and around the world. In this study, researchers will focus on the quality of postoperative recovery — at one day and at 30 days after surgery — as well as the incidence of unintended intraoperative awareness, a rare complication in which a patient briefly awakens during a procedure and becomes aware of what is happening.
“We see variations in patient experience on a daily basis — recovery from surgery and anesthesia can range from a few hours to a few months,” said Kheterpal, who also serves as the MPOG research director. “This study focuses on helping patients recover as quickly as possible so that they can get back to their daily lives, and we are thrilled to receive support from PCORI as we embark on this multicenter study because we believe this work has the potential to rapidly inform and improve perioperative patient care.”
The trial will include 12,500 adult patients undergoing elective, noncardiac surgery. Patients eligible to participate in the study will be invited prior to surgery. If they consent, they will be randomized to either intravenous propofol or inhaled anesthetic drugs.
Some patients will receive fitness trackers or smartwatches in the days or weeks prior to and after surgery so the researchers can obtain details regarding their standard levels of activity, heart rates, sleep patterns and other signals of health. Following surgery, all study patients will be provided with a smartphone app or a website link to submit information about their recoveries. Study personnel also will follow up with the patients for up to 90 days to monitor each patient’s recovery and related outcomes important to patients, such as postoperative delirium or confusion.
Twelve centers that are part of the MPOG group will serve as clinical sites. Those sites will be chosen to represent various geographic locations, and they will be a mix of academic and community health centers. Researchers expect to launch a 200-patient pilot study in the next several months, with the full 12,500-patient trial to follow.
This work is supported by the Patient-Centered Outcomes Research Institute (PCORI).
Washington University School of Medicine’s 1,700 faculty physicians also are the medical staff of Barnes-Jewish and St. Louis Children’s hospitals. The School of Medicine is a leader in medical research, teaching and patient care, consistently ranking among the top medical schools in the nation by U.S. News & World Report. Through its affiliations with Barnes-Jewish and St. Louis Children’s hospitals, the School of Medicine is linked to BJC HealthCare.



Comments and respectful dialogue are encouraged, but content will be moderated. Please, no personal attacks, obscenity or profanity, selling of commercial products, or endorsements of political candidates or positions. We reserve the right to remove any inappropriate comments. We also cannot address individual medical concerns or provide medical advice in this forum.