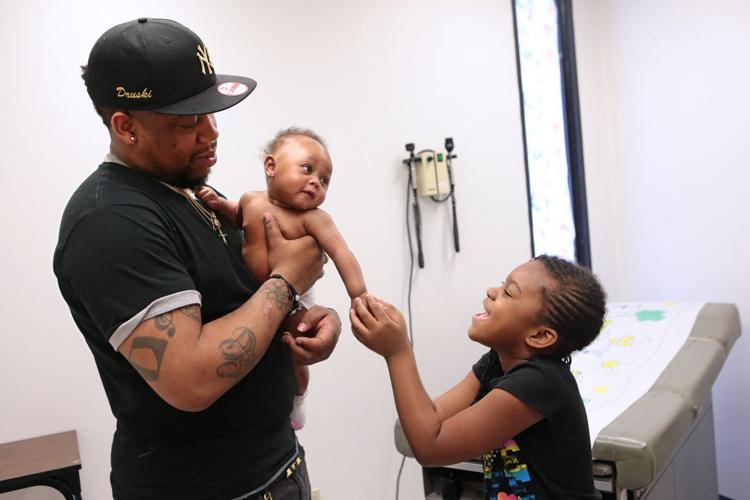
Andrew Scott waited Wednesday afternoon in the lobby of Affinia Healthcare with his three daughters. His youngest, 4-month-old Addisyn, was due for a checkup and vaccinations.
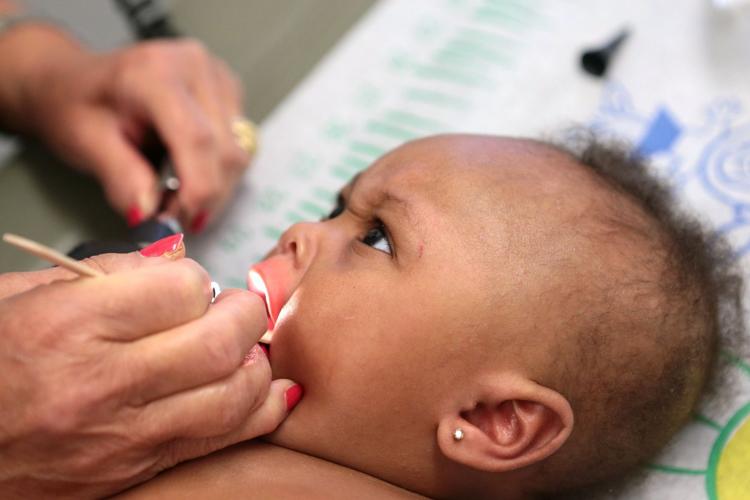
After getting weighed, measured and pricked, the babbling infant received a clean bill of health.
Medicaid pays for Addisyn’s visits at the St. Louis clinic. Her dad, however, isn’t eligible for the program. Though he’s struggling to get by, he makes too much money to qualify for the government health care program in Missouri.
Missouri has among the most restrictive Medicaid programs in the nation, in part, a consequence of the state refusing to expand the program under the Affordable Care Act.
And while Republican efforts to repeal and replace the law known as Obamacare fell short last week, health care analysts say pressure on the Medicaid program will continue. On Friday, House Speaker Paul Ryan pulled the American Health Care Act when Republicans were unable to muster enough votes to pass the bill.
People are also reading…
“Regardless of what happens ... with the AHCA, it is pretty clear that there is going to be changes with Medicaid under this administration,” said Matt Salo, executive director of the National Association of Medicaid Directors.
Those changes, proposed both in Washington and Jefferson City, could mean even fewer people qualifying for coverage — and that has health care providers, especially hospitals in some of the state’s poorer communities, worried.
The AHCA would have hit the Medicaid program the hardest through a $880 billion cut in funding, which would have resulted in 14 million fewer Medicaid enrollees nationwide, according to an estimate by the nonpartisan Congressional Budget Office.
In Missouri, with nearly 1 million Missourians who rely on Medicaid, about 306,500 people would have lost coverage under the original proposal, according to estimates from the Center for American Progress, a left-leaning policy institute in Washington, D.C.
The Republican goal was to control the rapid escalation in Medicaid spending fueled in large part by the Affordable Care Act, which was signed into law in 2010. In a 10-year period, from 2004 to 2014, total Medicaid expenditures have increased 71 percent, according to a November 2016 report from Standard & Poor’s.
Under the Republican proposal, the federal government would have placed a limit on how much was spent on each enrollee in the program instead of matching a certain percent of what the state spends.
But changing the program from a percentage match to a capped system could make states vulnerable to budget shortfalls, according to a November 2016 report from Standard & Poor’s.
A capped-funding formula for Medicaid could cause a domino effect that leads to cuts in both covered services and the number of enrollees in an effort to plug predicted shortages at the state level, according to the CBO.
And Missouri’s unique funding structure could lead to more extreme budget shortfalls, according to health care executives.
“It’s hard to envision that a capped reimbursement ... would not in some way or in some manner lower eligibility, restrict benefits and or reduce reimbursements to providers,” said Alan Freeman, CEO of Affinia Healthcare.
Forty-two percent of the patients at Freeman’s clinics rely on Medicaid to pay for health care services.
Who gets Medicaid?
To be eligible for Medicaid, Missourians must be poor and also fit into one of several specific categories: elderly, disabled, a child or pregnant. An extremely poor parent of a child in the program may also qualify in some cases.
For example, the child of a single mother could qualify for Medicaid as long as the mother’s annual income did not exceed $49,532. (The mother could be eligible if her annual income fell below $3,696.)
But an adult under 65 without children or a disability is not eligible — no matter how poor.
Unlike a majority of other states, Missouri lawmakers declined to expand Medicaid under Obamacare, which would have allowed adults without children to be eligible simply based on income.
Freeman worries funding changes will harm his most vulnerable patients with few means. He’s not alone in his opinion.
Map by Walker Moskop
Patrick Carron is the leader of a critical access hospital in Perry County, about 80 miles south of St. Louis. Carron’s hospital is the only one in the 19,000-person county. About 16 percent of Perry County residents rely on Medicaid, according to data from the Census Bureau and Missouri Department of Social Services.
If patients start losing Medicaid coverage and more become uninsured, Carron said it would create a ripple effect in his county, causing access problems for patients and financial strain for hospitals and a “hidden tax” on insurers and employers.
“It basically would correspond with an increase in our bad debt,” he said.
And when that happens it puts more pressure on his hospital to cut services or lean more heavily on those who can pay, like patients with commercial insurance — a “hidden tax,” he says.
But he’s also worried about changes to how the program is funded at the state level. Missouri is unique in using a tax on providers to fund most of the state’s portion of the program.
In Missouri, the federal government funds about 51 percent of the Medicaid program, the state’s general revenue funds 17 percent. The other 32 percent of funding is largely from taxes placed on providers and hospitals.
Any shake-up in that equation would leave the state on the hook for “spending considerably more,” Carron said.
Missouri’s Medicaid program largely benefits children from low-income and working-class homes. At about 63 percent of total enrollment, children represent the largest demographic insured by the program.
But while Missouri’s children make up most of the enrollment, most of the spending is driven by the elderly and those with disabilities, who make up just 25 percent of enrollees, according to Missouri Department of Social Services.
About 63 percent of nursing homes are funded with Medicaid dollars, according to the Missouri Foundation for Health.
About 71 percent of the patients served at St. Francis Medical Center in Cape Girardeau are covered either by Medicaid or Medicare, the government program for Americans age 65 and over. Had the GOP plan been enacted, St. Francis would have lost an estimated $152 million in Medicaid payments over the next 10 years, said CEO Steve Bjelich.
“Health care is pretty resilient but the economic implications of this round of reductions has never been seen to this level before and that should be a concern to all Missourians and all Americans,” he said.
Jefferson City weighs in
Proposed changes to the Medicaid program are also brewing in Jefferson City. Sen. David Sater, R-Cassville, wants a work requirement and he also wants enrollees to be on the hook for copays and premiums. His bill also seeks federal funding caps, a popular idea among Republicans.
Tim McBride, a health care economist at Washington University, said there’s already discussion in Jefferson City about “transforming” Missouri’s Medicaid program. And even though the AHCA failed to get enough support for a vote late last week, parallel changes will be pursued in the Republican-led Legislature.
The Medicaid work requirement is among the state proposals that could get the green light from the Trump administration, McBride says.
Critics promise a fight.
“We need to debunk the myth of who is on Medicaid in Missouri,” said Joe Pierle, CEO of Missouri’s Primary Care Association, which represents Missouri’s community health centers like Affinia.
“Does it make sense to impose work requirements on disabled, elderly and children that comprise Missouri’s Medicaid program?” Pierle asked.