Study reverses thinking on genetic links to stress, depression
New research led by the School of Medicine shows that an influential 2003 study about the interaction of genes, environment and depression may have missed the mark.
Higher blood levels of omega-3 may help depression in heart patients
New research at the School of Medicine indicates that initial levels of omega-3 fatty acids in a heart patient’s blood have a significant impact on whether that person will respond to omega-3 supplements to treat depression.
Two-drug combo helps older adults with hard-to-treat depression
More than half of older adults with clinical depression don’t get better when treated with an antidepressant. But results from a multicenter clinical trial that included Washington University School of Medicine in St. Louis indicates that adding a second drug — an antipsychotic medication — to the treatment regimen helps many of those patients.
Reward, aversion behaviors activated through same brain pathways
New research may help explain why drug treatments for addiction and depression don’t work for some patients. The conditions are linked to reward and aversion responses in the brain. And the research suggests that some treatments simultaneously stimulate reward and aversion responses, resulting in a net zero effect.
Device delivers drugs to brain via remote control
A team of researchers, including neuroscientists from Washington University School of Medicine in St. Louis, has developed a wireless device the width of a human hair that can be implanted in the brain and activated by remote control to deliver drugs to brain cells. The technology, demonstrated for the first time in mice, one day may be used to treat pain, depression, epilepsy and other neurological disorders in people by targeting therapies to specific brain circuits.
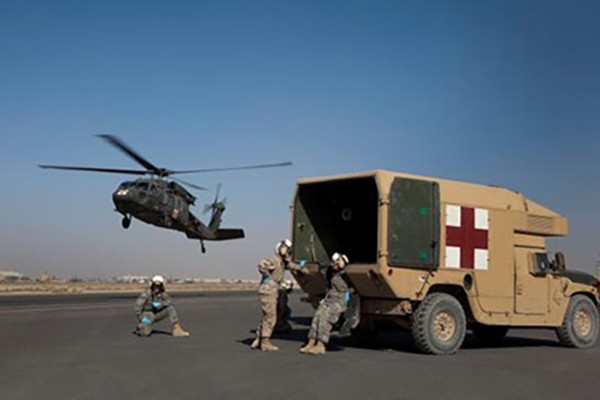
Mental health soon after war-zone concussions predicts disability
Evaluating military personnel with blast-related mild traumatic brain injuries, researchers have found that early symptoms of post-traumatic stress, such as anxiety, emotional numbness, flashbacks and irritability, are the strongest predictors of later disability. The study was led by the School of Medicine.
Depression, behavioral changes may precede memory loss in Alzheimer’s
Depression and behavioral changes may occur before memory declines in people who will go on to develop Alzheimer’s disease, according to new research at the School of Medicine led by senior author Catherine M. Roe, PhD.
Laughing gas studied as depression treatment
Nitrous oxide, or laughing gas, has shown early promise as a treatment for severe depression in patients whose symptoms don’t respond to standard therapies, according to a small pilot study led by (from left) psychiatrists Charles R. Conway, MD, and Charles F. Zorumski, MD, and anesthesiologist Peter Nagele, MD, at the School of Medicine.
Depression, overwhelming guilt in preschool years linked to brain changes
In school-age children previously diagnosed with depression as preschoolers, a key brain region involved in emotion is smaller than in their peers who were not depressed, scientists at the School of Medicine have shown.
Many depressed preschoolers still suffer in later school years
Children diagnosed with depression as preschoolers are likely to suffer from depression as school-age children and young adolescents, research shows. Depressed preschoolers were 2.5 times more likely to suffer from depression in later school years than children who were not depressed at very young ages, according to School of Medicine researchers.
View More Stories