A new tool to study Huntington’s disease
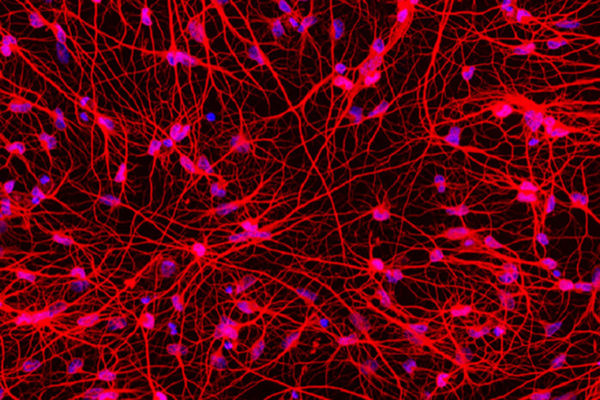
Scientists at the School of Medicine have transformed skin cells from patients with Huntington’s disease into the type of brain cell affected by the disorder. This offers a new tool to study the degenerative and eventually fatal neurological condition.
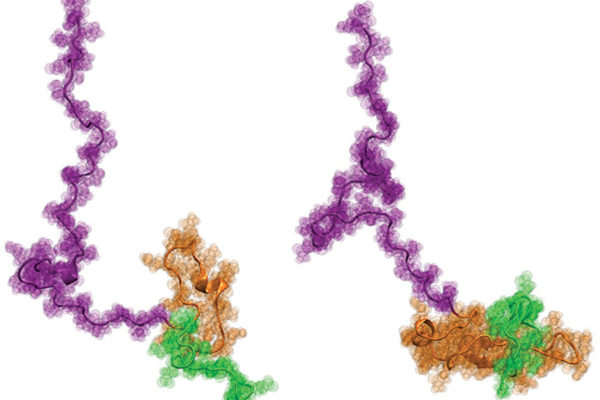
Imaging a killer
An international team of researchers has obtained the first ever atom-level structural insights into Httex1, a part of the gene that is thought to cause the devastating neurological disorder Huntington’s disease.
Drug compound halts Alzheimer’s-related damage in mice
Researchers at the School of Medicine have shown that levels of tau protein can be reduced – and some of the neurological damage caused by tau even reversed – by a synthetic molecule that targets genetic instructions. The findings are important for Alzheimer’s and other neurological diseases.
Huntington’s Disease target of $4.5 million in NIH grants
Rohit V. Pappu, the Edwin H. Murty Professor of Engineering in the School of Engineering & Applied Science at Washington University in St. Louis, has received two grants from the National Institutes of Health totaling more than $4.5 million to study the causes behind Huntington’s disease that may ultimately provide clues for a treatment or cure.
Human skin cells reprogrammed directly into brain cells
School of Medicine scientists have described a way to convert human skin
cells directly into a specific type of brain cell affected by
Huntington’s disease, an ultimately fatal neurodegenerative disorder.
Unlike other techniques that turn one cell type into another, this new
process does not pass through a stem cell phase, avoiding the production
of multiple cell types.
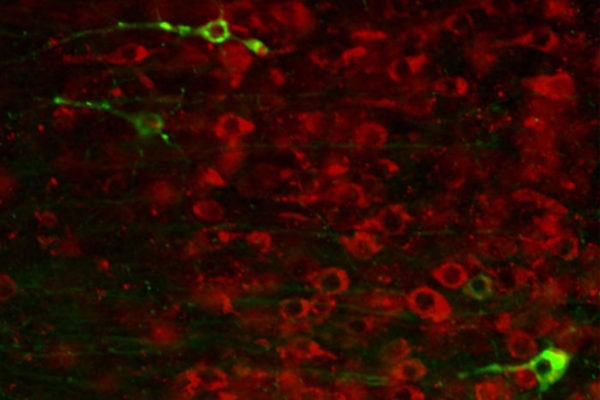
Fatal cell malfunction ID’d in Huntington’s disease
New research from the School of Medicine’s Albert Kim, MD, PhD (left), and Hiroko Yano, PhD, helps explain how mutations in the gene that causes Huntington’s disease kill brain cells. The findings could open new opportunities for treating the fatal disorder.
Staying ahead of Huntington’s disease
Huntington’s disease is a devastating, incurable disorder that results from the death of certain neurons in the brain. Rohit Pappu, PhD, and colleagues in the engineering and medical schools are conducting studies to learn from nature’s own strategies to battle the disease.