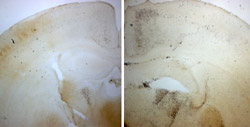
Can you blame your genes if you can’t handle your liquor? A new study conducted at Washington University School of Medicine in St. Louis may pave the way to finding out.
Researchers found that the brain’s response to alcohol is partially under the influence of two genes. The genes, studied in both adult and newborn mice, were found to affect sensitivity to alcohol intoxication, interest in alcohol consumption and risk of developmental brain damage from alcohol.
“Now that we understand that these genes are involved in neural processes affected by alcohol, we think they will be good candidates to look at in the human population,” says Louis Muglia, M.D., Ph.D., associate professor of pediatrics, of molecular biology and pharmacology and of obstetrics and gynecology. “It will be interesting to see if there are human variants of the genes associated with either fetal alcohol syndrome or addictive behaviors in adults.”
To uncover the genes’ effect, the research team — led by Muglia, also a pediatric endocrinologist at St. Louis Children’s Hospital — inactivated the two genes in mice.
In newborn mice with the genetic inactivation, ethanol (the alcohol used in beer, wine and spirits) caused significantly more neurodegeneration than it did in normal newborn mice. In adult mice with the genetic inactivation, the sedative effect of ethanol lasted up to twice as long. Further, when ethanol was freely available, adult mice with the inactivation drank much less ethanol than normal animals.
The researchers report their findings in two articles appearing in the March 2 and April 20 issues of the Journal of Neuroscience. James W. Maas, predoctoral trainee, is first author on both studies.
The genes studied make enzymes called adenylyl cyclases (AC), which support neural function and contribute to learning and memory. These enzymes are so essential that they exist in ten similar forms, and some type of AC is found in every cell of the body.
Two forms, AC1 and AC8, are found mainly in neurons. The researchers eliminated AC1 and AC8 from the brains of the mice by inactivating the genes that code for the enzymes.

“We wanted to test how the lack of AC1 and AC8 would influence ethanol-induced neurodegeneration in the brains of newborn mice—as a model for what happens in fetal alcohol syndrome in humans—and also how it would affect adult mice that consumed ethanol,” Muglia says.
Fetal alcohol exposure is regarded as the leading cause of mental and physical birth defects and is the most common preventable cause of birth defects in the United States. During the first week after birth, the brains of mice are in a stage of development similar to that of human fetuses during the last trimester of pregnancy.
The research team found that in the newborn mice, the lack of AC1 and AC8 increased neuronal sensitivity to ethanol’s destructive effects. Newborn mice missing either of the AC enzymes and given ethanol had much greater neuronal damage, even at low ethanol doses, than normal mice.
“If you look at children who were exposed to alcohol during gestation, you’ll see that not all develop fetal alcohol syndrome,” Maas says. “We think the levels of AC1 and AC8 enzymes may predispose a fetus to being more or less sensitive to alcohol consumption by the mother.”
Theorizing that the enzymes modulating ethanol’s effect during brain development might be the same ones involved in ethanol actions later in life, the researchers looked at the effects of the same genetic inactivations in adult mice.
In adult mice, ethanol does not damage neurons in the brain, but it does have a marked sedative effect. The studies showed that adult mice lacking AC1 slept 1.5 to 2 times longer for a given ethanol dose than normal mice. The researchers did not see that effect in mice lacking AC8.
Previous studies have shown that the more sensitive an animal is to sedation by ethanol, the less ethanol it seeks to drink. Mice lacking AC8, but not those lacking AC1, displayed significantly lower preference for ethanol and cut their voluntary ethanol consumption compared to normal mice.
In contrast, mice lacking the enzymes suffered the same amount of ataxia, or loss of muscle coordination, after ethanol consumption as normal mice.
“Our results confirm that ethanol affects various parts of the adult brain via different mechanisms,” Muglia says. “Ataxia deficits are thought to be mediated primarily by the cerebellum. Because ataxia after ethanol consumption was the same in both altered and normal mice, AC1 and AC8 probably are not critical to ethanol’s effects in the cerebellum. But, the effects on sedation and ethanol preference suggest that each AC gene has a role in influencing ethanol’s effects in the cerebral cortex.”
The studies demonstrated that the response to ethanol is very different in newborn compared to adult mice.
“During development, the brain makes more neurons than it needs and weeds out unnecessary neurons by killing the inactive ones. In adults, however, the brain wants to protect all its neurons,” Muglia says. “By blocking neuronal receptors, ethanol exaggerates the normal destruction of neurons in the developing brain, but it only temporarily turns off neurons in the adult brain. AC1 and AC8 help mediate these processes.”
Mass JW Jr, Vogt SK, Chan GCK, Pineda VV, Storm DR, Muglia LJ. Calcium-stimulated adenylyl cyclases are critical modulators of neuronal ethanol sensitivity. Journal of Neuroscience, 2005 April 20;25(16):4118-4126.
Mass JW Jr, Indacochea RA, Muglia LM, Tran TT, Vogt SK, West T, Benz A, Shute AA, Holtzman DM, Mennerick S, Olney JW, Muglia LJ. Calcium-stimulated adenylyl cyclases modulate ethanol-induced neurodegeneration in the neonatal brain. Journal of Neuroscience, 2005 March 2;25(9):2376-2185.
Funding from the National Institutes of Health and the Washington University Medical Scientist Training Program supported this research.
Washington University School of Medicines full-time and volunteer faculty physicians also are the medical staff of Barnes-Jewish and St. Louis Children’s hospitals. The School of Medicine is one of the leading medical research, teaching and patient care institutions in the nation, currently ranked third in the nation by U.S. News & World Report. Through its affiliations with Barnes-Jewish and St. Louis Children’s hospitals, the School of Medicine is linked to BJC HealthCare.