Despite decades of research and investment, the genetic underpinnings of Alzheimer’s disease are still largely unknown, stymieing efforts at drug development and early diagnosis. To change that, a new grant will support the first comprehensive study to use whole genome sequencing to address critical gaps in knowledge about the disease. The $10.7 million, five-year project is led by researchers at Washington University School of Medicine in St. Louis and the University of Pittsburgh Graduate School of Public Health.
Funded by the National Institute on Aging of the National Institutes of Health (NIH), the research team plans to identify the genetic variants, genes and pathways that lead to formation of plaques and tangles, two specific signs of disease — called biomarkers — that begin appearing in the brains of people with Alzheimer’s 15 to 25 years before they show symptoms.

“Genetic studies of measurable traits such as plaques and tangles provide advantages over other classic case-control studies, because these traits appear earlier and are more closely related to the biology behind the disease,” said Carlos Cruchaga, a co-principal investigator of the study and the Reuben Morriss III Professor of Neurology at Washington University School of Medicine. “In addition, studying these traits is more likely to lead to the identification of druggable targets along the genetic pathways that lead to disease. This genetic information can help us better predict disease risk at the individual patient level.”
Cruchaga, also a professor of psychiatry, is working with co-principal investigator Ilyas Kamboh, professor of human genetics and epidemiology at Pitt Public Health. Together, they plan to study as many as 5,000 participants at high risk for Alzheimer’s. The researchers will gather biomarker data to identify genetic variants that appear decades before clinical symptoms of the disease.
“All of the clinical trials to find a drug to stop Alzheimer’s disease have failed because they’ve focused on patients who already have developed the disease, so they already had high levels of plaques and tangles,” said Kamboh. “Once you have the plaques and tangles, it seems to be an irreversible process, so we’re focused on the preclinical stage of the disease.”
According to the World Health Organization, Alzheimer’s disease is the most common form of dementia, with about 50 million cases worldwide and 6 million new cases each year. It is one of the major causes of disability and dependency among older people.
The plaques and tangles in the brain associated with Alzheimer’s can be thought of like cholesterol in the arteries of the heart and its association with heart disease, Kamboh explained. Cholesterol can quietly accumulate over years along the walls of the coronary arteries without causing symptoms until it causes a heart attack and does irreversible damage to the heart. Some genes predispose people to accumulate more cholesterol, and understanding that can allow people to take medication and make lifestyle changes that reduce the risk of heart disease. It also can prompt pharmaceutical companies to develop drugs that target the genetic pathways that lead to the formation of cholesterol deposits.
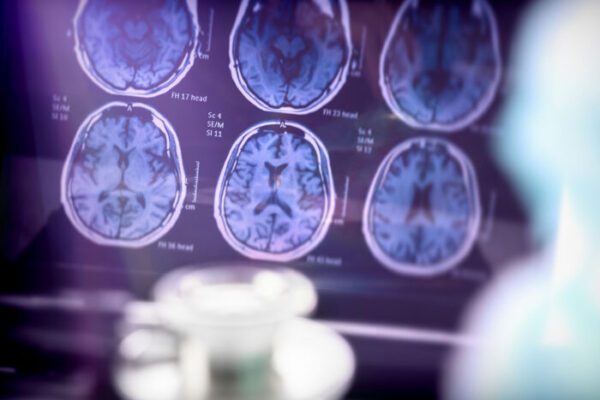
The new project will look for the genetic underpinnings of the plaques and tangles known to define Alzheimer’s disease and that formed due to abnormal accumulation of amyloid beta and tau proteins, respectively. Both can be detected early in the brains of living people through neuroimaging and the testing of cerebrospinal fluid.
“In the past, we could detect these plaques and tangles only after death, through a brain autopsy,” Kamboh said. “Now we can identify them while people are living.”
But those imaging and fluid-collection techniques are expensive and can be invasive.
“New methods are now being developed to detect the presence of abnormal amyloid beta and tau proteins in less expensive blood tests,” Cruchaga said. “We hope that by learning more about the genes associated with the plaques and tangles, we might uncover underlying pathways that lead to Alzheimer’s disease and discover potential drug targets.”
This study is supported by the National Institute on Aging of the National Institutes of Health (NIH). Grant number R01 AG064877.
Washington University School of Medicine’s 1,500 faculty physicians also are the medical staff of Barnes-Jewish and St. Louis Children’s hospitals. The School of Medicine is a leader in medical research, teaching and patient care, consistently ranking among the top medical schools in the nation by U.S. News & World Report. Through its affiliations with Barnes-Jewish and St. Louis Children’s hospitals, the School of Medicine is linked to BJC HealthCare.