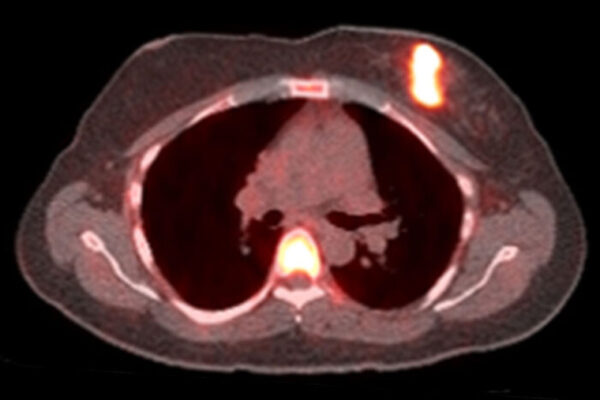
Immunotherapy has transformed cancer care. In advanced melanoma, for example, the most fatal form of skin cancer, the five-year survival rate has risen from less than 10% to more than 50% since immunotherapy was introduced in 2011. Still, only about half of melanoma patients respond to immunotherapy, and those who do not respond face a difficult future.
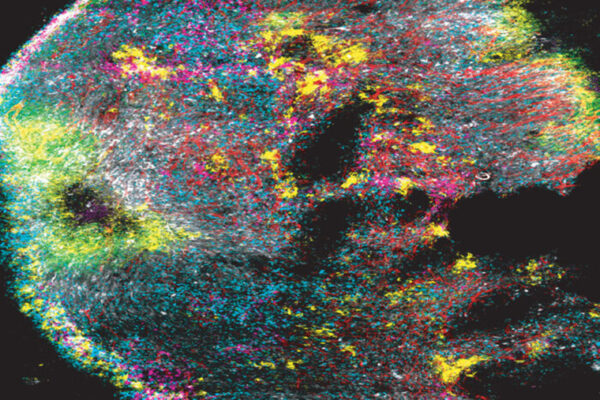
Researchers at Washington University School of Medicine in St. Louis have discovered that the difference between people who do and do not respond to immunotherapy may have to do with an immune cell known as CD5+ dendritic cells because they bear the protein CD5 on their outer surfaces. Their research showed that people with a variety of kinds of cancers, including melanoma, lived longer if they had more CD5+ dendritic cells in their tumors, and that mice that lacked CD5 on their dendritic cells were unable to respond well to immunotherapy.
The findings, published Feb. 17 in the journal Science, suggest that a supplementary therapy designed to increase the number or activity of CD5+ dendritic cells potentially could extend the lifesaving benefits of immunotherapy to more cancer patients.
“Immunotherapy has revolutionized the field of cancer therapy, but there are a lot of patients with cancer who don’t benefit from it,” said senior author Eynav Klechevsky, PhD, an assistant professor of pathology & immunology and a researcher at Siteman Cancer Center at Barnes-Jewish Hospital and Washington University School of Medicine. “Part of the reason some people do not respond well to some forms of immunotherapy is because this population of dendritic cells is reduced dramatically. We’re developing some novel immune-based approaches to boost the activation of these CD5-expressing dendritic cells with a goal of helping more patients respond to immunotherapy.”
The immune system defends the body against cancer by activating immune cells known as T cells to recognize and kill tumor cells. In response, tumor cells manipulate the immune checkpoint system — a safeguard that prevents T cells from mistakenly attacking healthy cells — to hoodwink T cells into leaving them alone. Immune checkpoint blockade therapy works by thwarting tumor cells’ manipulations, thereby freeing T cells to recognize and destroy tumors. But even with therapy, some people’s T cells are unable to do their job effectively.
Klechevsky and colleagues — including first author Mingyu He, PhD, a staff scientist, and co-author Kate Roussak, MD, a postdoctoral researcher — suspected that people who don’t respond to immunotherapy may have a problem with their dendritic cells. If T cells are the players on a soccer field, dendritic cells are the coaches who get the players pumped up for the game and give them instructions. Without dendritic cells, T cells are subdued and aimless.
By analyzing data in The Cancer Genome Atlas — a public database with information on 20,000 tumors representing 33 cancer types — Klechevsky and colleagues discovered that patients with types of skin, lung, bone and soft tissue, breast and cervical cancers fared better if they had higher levels of CD5+ dendritic cells in their tumors.
Further experiments with human cells and mice showed that CD5+ dendritic cells are required for effective T cell activity against tumors. CD5+ dendritic cells from people powerfully induced T cells to activate and multiply. Mice with tumors responded only weakly to immunotherapy and failed to reject the tumors if they lacked CD5 on their dendritic cells.
The findings suggest that the amount of CD5+ dendritic cells inside tumors could be used to help doctors assess which patients are most likely to benefit from immunotherapy. They also suggest that increasing the numbers or the activity of such dendritic cells potentially could help more people benefit from immunotherapy. As part of this study, the researchers discovered that the immune protein IL-6 increases the amounts of CD5+ dendritic cells.
“We still don’t completely understand how immunotherapies work,” Klechevsky said. “This study indicates that there is more we can do to increase the efficacy of these treatments. I’m confident that if we can find ways to harness these cells or expand these cells in patients, we can help more people.”
He M, Roussak K, Ma F, Borcherding N, Garin V, White M, Schutt C, Jensen TI, Zhao Y, Iberg CA, Shah K, Bhatia H, Korenfeld D, Dinkel S, Gray J, Ulezko Antonova A, Ferris S, Donermeyer D, Lindestam Arlehamm C, Gubin MM, Luo J, Gorvel L, Pelligrini M, Sette A, Tung T, Bak R, Modlin RL, Fields RC, Schreiber RD, Allen PM, Klechevsky E. CD5 expression by dendritic cells directs T cell immunity and sustains immunotherapy responses. Science. Feb. 17, 2023. DOI: 10.1126/science.abg2752
This work was funded by the National Institutes of Health (NIH), grant numbers 1R01CA245277-01A1, 5R01AR075959-02, 5R21EB024767-03, T32 CA009547-34, R01 AI022553, R01 AR040312, R01 AR073252, R01 AR074302, R01 AI166313, and P50 AR080594; the National Psoriasis Foundation; Novo Nordisk, grant number NNF17OC0028894.
About Washington University School of Medicine
WashU Medicine is a global leader in academic medicine, including biomedical research, patient care and educational programs with 2,700 faculty. Its National Institutes of Health (NIH) research funding portfolio is the third largest among U.S. medical schools, has grown 54% in the last five years, and, together with institutional investment, WashU Medicine commits well over $1 billion annually to basic and clinical research innovation and training. Its faculty practice is consistently within the top five in the country, with more than 1,800 faculty physicians practicing at 65 locations and who are also the medical staffs of Barnes-Jewish and St. Louis Children’s hospitals of BJC HealthCare. WashU Medicine has a storied history in MD/PhD training, recently dedicated $100 million to scholarships and curriculum renewal for its medical students, and is home to top-notch training programs in every medical subspecialty as well as physical therapy, occupational therapy, and audiology and communications sciences.