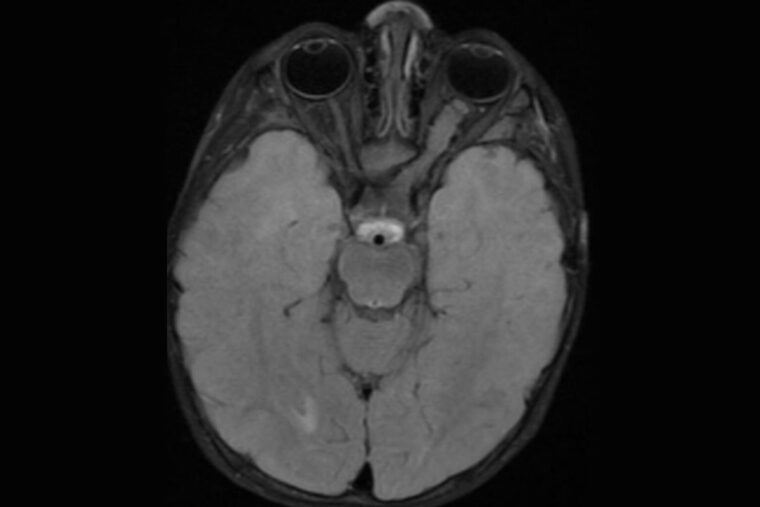
A drug used to treat children with epilepsy prevents brain tumor formation and growth in two mouse models of neurofibromatosis type 1 (NF1), according to a study by researchers at Washington University School of Medicine in St. Louis. NF1 is a genetic condition that causes tumors to grow on nerves throughout the body, including the optic nerves, which connect the eyes to the brain.
The findings lay the groundwork for a clinical trial to assess whether the drug, lamotrigine, can prevent or delay brain tumors in children with NF1. The study is online in the journal Neuro-Oncology.
“Based on these data, the Neurofibromatosis Clinical Trials Consortium is considering launching a first-of-its-kind prevention trial,” said senior author David H. Gutmann, MD, PhD, the Donald O. Schnuck Family Professor of Neurology and the director of Washington University’s Neurofibromatosis Center. The clinical trials consortium is an international network of NF scientists that was formed by the U.S. Department of Defense in 2006 to find therapies for all forms of neurofibromatosis. “The plan is to enroll kids without symptoms, treat them for a limited time, and then see whether the number of children who develop tumors that require treatment goes down.
“This is a novel idea, so we took it to an NF1 patient focus group,” Gutmann continued. “They said, ‘This is exactly what we’re looking for.’ A short-term treatment with a drug that has been used safely for 30 years was acceptable to them if it reduced the chance their children would develop tumors and need chemotherapy that might have all kinds of side effects.”
The most serious tumors that people with NF1 get affect the optic nerve and are known as optic gliomas. Such tumors typically appear between ages 3 to 7. While they are rarely fatal, they cause vision loss in up to a third of patients as well as other symptoms, including early puberty. Standard chemotherapy for optic gliomas is only moderately effective at preventing further vision loss and can affect children’s developing brains, resulting in cognitive and behavioral problems.
In a previous study, Gutmann and Corina Anastasaki, PhD, an assistant professor of neurology and the first author on the new paper, showed that lamotrigine stopped optic glioma growth in NF1 mice by suppressing neuronal hyperactivity. The Neurofibromatosis Clinical Trial Consortium found their data intriguing but demanded more evidence before they would consider launching a clinical trial. The consortium members asked Gutmann and Anastasaki to clarify the connection between Nf1 mutation, neuronal excitability and optic gliomas; assess whether lamotrigine was effective at the doses already proven safe in children with epilepsy; and conduct these studies in more than one strain of NF1 mice.
In people, NF1 is a highly variable disease. It can be caused by any one of thousands of different mutations in the NF1 gene, where different mutations could be associated with different medical problems. Repeating experiments in multiple strains of mice was a way of gauging whether lamotrigine was likely to work in people regardless of the underlying mutation.
Anastasaki and Gutmann not only showed that lamotrigine worked in two strains of NF1 mice, they also showed that the drug worked at lower doses than those used for epilepsy, meaning that it was probably safe. Even better, they found that a short course of the drug had lasting effects, both as a preventive and a treatment. Mice that had tumors and that were treated for four weeks starting at 12 weeks of age saw their tumors stop growing and even showed no further damage to the retinas of their eyes. Mice that received a four-week course of the drug starting at 4 weeks of age, before tumors typically emerge, showed no tumor growth even four months after treatment had ended.
These findings have led Gutmann to suggest that a one-year course of treatment for young children with NF1, maybe between the ages of 2 to 4, might be enough to reduce their risk of brain tumors.
“The idea that we might be able to change the prognosis for these kids by intervening within a short time window is so exciting,” Gutmann said. “If we could just get them past the age when these tumors typically form, past age 7, they may never need treatment. I’d love it if I never again had to discuss chemotherapy for kids who aren’t even in first grade yet.”
Anastasaki C, Chatterjee J, Koleske JP, Gao Y, Bozeman SL, Kernan CM, Marco Y Marquez LI, Chen JK, Kelly CE, Blair CJ, Dietzen DJ, Kesterson RA, Gutmann DH. NF1 mutation-driven neuronal hyperexcitability sets a threshold for tumorigenesis and therapeutic targeting of murine optic glioma. Neuro-Oncology. April 12, 2024. DOI: 10.1093/neuonc/noae054
This work was funded by the Giorgio Foundation; the National Cancer Institute of the National Institutes of Health (NIH), grant number R01CA258384 and R50CA233164; the National Institute of Neurological Disorders and Stroke of the NIH, grant number R35NS097211; and the Gilbert Family Foundation. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
About Washington University School of Medicine
WashU Medicine is a global leader in academic medicine, including biomedical research, patient care and educational programs with 2,900 faculty. Its National Institutes of Health (NIH) research funding portfolio is the second largest among U.S. medical schools and has grown 56% in the last seven years. Together with institutional investment, WashU Medicine commits well over $1 billion annually to basic and clinical research innovation and training. Its faculty practice is consistently within the top five in the country, with more than 1,900 faculty physicians practicing at 130 locations and who are also the medical staffs of Barnes-Jewish and St. Louis Children’s hospitals of BJC HealthCare. WashU Medicine has a storied history in MD/PhD training, recently dedicated $100 million to scholarships and curriculum renewal for its medical students, and is home to top-notch training programs in every medical subspecialty as well as physical therapy, occupational therapy, and audiology and communications sciences.
Originally published on the School of Medicine website